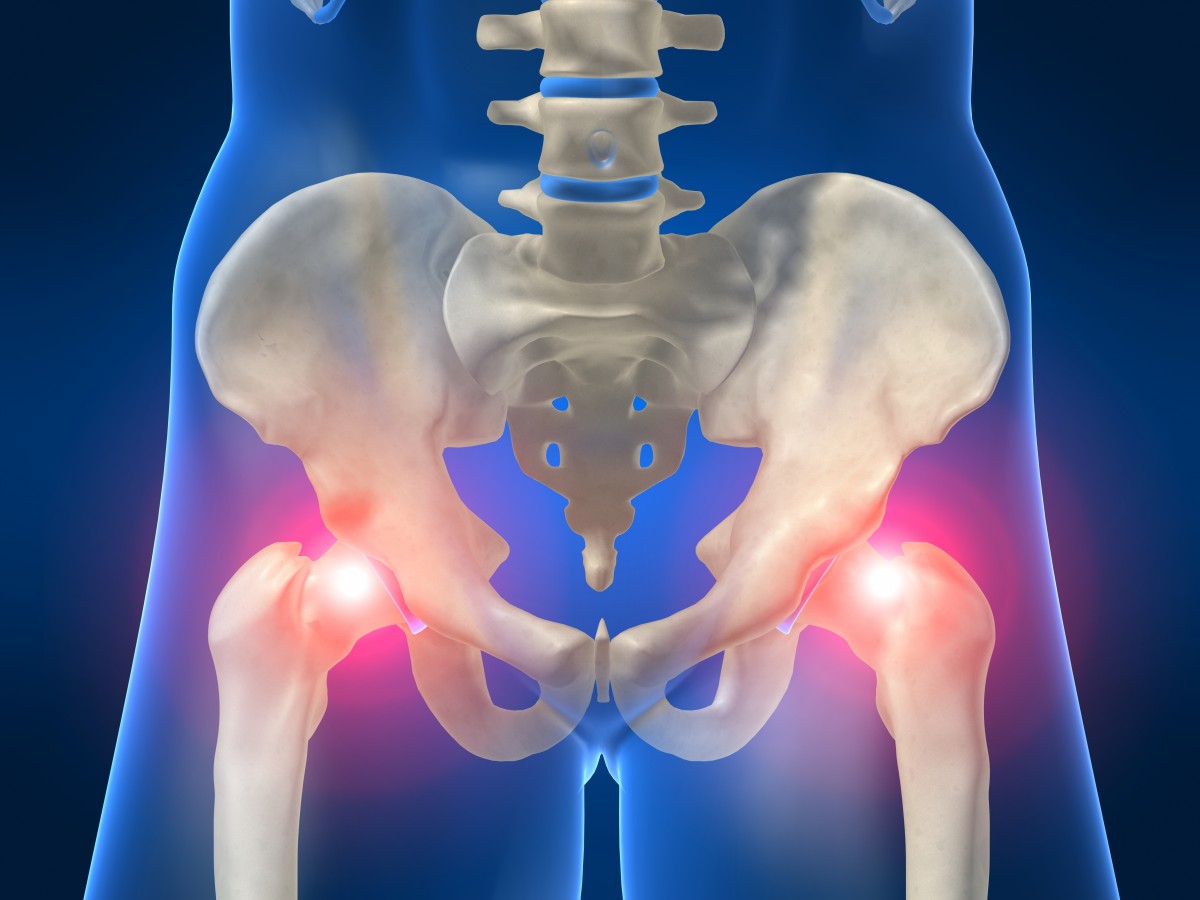
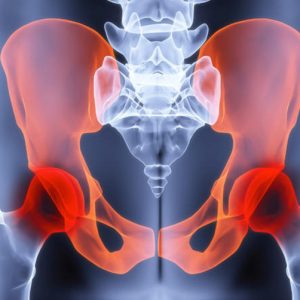
Pain below the umbilicus to the groin is called pelvic pain. Women are usually more likely than men to have chronic pelvic pain, which can have a variety of causes, ranging from minor disorders to serious disorders that require follow-up.
تیترهای مهم این مقاله
Visceral pains of the female organs
Benign etiology of pelvic pains include ovulation pain, premenstrual syndrome, genital infections, and uterine structural problems such as fibroids and uterine masses. One of the major causes of benign problems of the female is endometriosis that in many cases it needs to be treated interventionally.
Endometriosis is a disorder in which tissue like endometrium tissues placed in other organs. It may occur on the surface of the ovary, behind the uterus, and in the pelvic cavity, on the intestinal wall, and rarely in distant locations. Increasing pelvic pain during menstruation, pain during intercourse, spotting before menstruation, sometimes blood in the urine or stool, low back pain and intestinal contractions are one of the symptoms and one of the best treatments is the supriorhypogastric plexus block.
Visceral pain of kidneys, bladder and urinary tract
Infections, stones, and any abnormalities of the urinary tract involve any part of the urinary tract from the bladder to the urinary tract and the kidneys. Symptoms of this disease include pressure on the lower pelvis, pain when urination , and even gastrointestinal symptoms.
If all the related problems have been resolved by the relevant specialists and the pain has remained chronic, nerve block and radiofrequency of hypogastric plexus and other necessary techniques can be used .
Pelvic wall pain
Inguinal hernia can cause pelvic pain,it is more common in pregnant women because of the increased abdominal pressure . Also in the repair of the hernia wall, there are many people with parietal pain that require interventional pain treatments such as the ilioinguinal and iliohypogastric nerve blocks.
Spinal problems
Back pain and spine can be felt in the pelvis and in the seat. Sciatica also causes pain in the back of the pelvis, which is explained in more detail in other parts.
Pelvic Skeletal Problems
One of the most common problems that need to be treated interventionally. The hip joint is a very stable and mobile joint. Pelvic ligaments and muscles help stabilize the pelvis.
Hip
Repeated trauma can make joint painful. Joint inflammatory diseases (rheumatoid arthritis and arthrosis) and lack of blood perfusion to the femoral head are the most common causes of pelvic pain. Hip pain is felt in the groin, hip, outer part of the thigh or knee. Labrum cartilage damage and frequent tearing cause crepitation and pain.
Tendon and muscle problems
The buttock muscles(Ghuteous ..) play an important role in stabilizing the joint. If the muscles around the pelvis do not support it well, in addition to buttock and hip pain, there is the problem of stretching of the muscles and tendons, also known as tendinopathy.
Tendon inflammation and bursitis
Many tendons around the pelvis connect the muscles to the joint. These tendons are easily inflamed by exercise or heavy activity. Another common cause of pelvic pain is inflammation. Bursitis is an inflammation of the fluid-filled sac that protects the bony part of the pelvis. These bags, like tendons, become inflamed by overuse or discomfort and cause pelvic pain when moving. The most com mon and annoying type of bursitis is trochanteric bursitis, a painful complication that occurs near or near the larger trochanter.
Sacroiliac Joint Pain
Osteoarthritis and inflammation of the joint connecting the sacrum to the pelvis can cause severe pain in the pelvic region.
Piriformis and Psoas Muscle Spasms
Psoas and piriformis are the deep pelvic stabilizer muscle that attaches to the spine above the femur.Psoas and quadratus lumburum spasm can causes spastic pain in the lumbar spine.Spasm of piriformis is the consequence of inflammation of the muscle that causes pressure on the sciatic nerve, which in turn causes sciatic nerve and pain in the pelvis and diffuse pain in the leg.
Diagnosis of pelvic pain
Physical examination and evaluation of muscle reflexes and gait are important.
- Imaging : Imaging tests provide the physician with complete information about the pelvic structure and problems, including:
- Pelvic X-ray : To evaluate the pelvic bone tissue
- Computed tomography : CT scans can be used for more evaluation.
- MRI : Used to examine soft tissues including the viscera, pelvic muscles, spinal cord and nerves.
- Laboratory Test : Blood tests are very helpful in diagnosing inflammatory causes.
Treatment of chronic pelvic pain
The treatment depends on the patient’s symptoms. The therapies are step by step, and if the patient does not respond appropriately to each treatment step, more sophisticated methods are used.
Rest : The patient is advised to avoid repeated hip flexion and direct pressure on the hip. It will not tilt to the painful side and will not sit for long.
Medication : Medications are used to relieve symptoms in the acute phase as well as to restore muscle strength and relaxation, including: muscle relaxants, anti-inflammatory analgesics, and soy and avocado combination drugs can be used to prevent the progression and recovery of arthritic lesions.
Heat or cold therapy : Put a few pieces of ice wrapped in towels over a painful hip. Conversely, a shower or hot water bath also prepares muscles for stretching exercises to reduce pain by doing these exercises.
Non-invasive treatments for chronic pelvic pain
Physiotherapy : In physiotherapy, a combination of passive techniques and exercises is used to strengthen muscular structure and corrective movements. Passive therapeutic modalities such as ice / heat, ultrasound and electrical stimulation reduce pain and spasm in the patient. With the help of specific exercises, the patient learns to increase flexibility and range of motion and increase his or her muscle strength. Patients should not worry about switching to this treatment, even patients with pain and movement problems benefit from isometric exercises.
Massage Manipulation : The basis of these techniques performed by hand also strengthens the muscle structure of the tissues.
High Power laser : The use of high-power pulse laser will increase cellular energy and repair damaged tissues and prevent the progression of arthritis.
Interventional treatments
Interventional procedures are performed by a pain specialist under the guidance of X-ray (fluoroscopy) or ultrasound in the operating room.
Diagnostic and therapeutic injections :
Injections into the pelvic problematic joints such as ozone, platelet, orthokine, etc., can stop the inflammation of the arthritic area. Radiofrequency in these areas can be used for long-term changes in addition to injections. Other Intervention methods can also be used, which are described in more detail in other sections and articles.